About Us
At InfoMC, we believe it is possible to directly improve healthcare delivery, reduce costs and optimize outcomes through the use of technology. It is this belief that motivates us to develop innovative, state of the art utilization and care management technology designed to enable care teams to address physical and behavioral health conditions, social determinants of health and long term services and support needs, for high-risk and specialty populations.
How it Started
InfoMC got its start in 1995 by launching an enterprise platform to manage all clinical and core administration functions for a Philadelphia-based managed behavioral health organization. Shortly after, the platform was expanded to also support Employee Assistance Programs adding community referrals and scheduling. This solidified InfoMC’s position in the world of behavioral healthcare for years to come.
Inspired by his vision of improving healthcare, InfoMC CEO, JJ Farook, saw significant value in expanding beyond our behavioral health solution to create a whole-person, integrated care platform. By 2013, this led InfoMC’s transition to providing a cloud-based care management, utilization management and care coordination solution – supporting behavioral, physical and community-based services – known as the Incedo™ Healthcare Management System.


How it Started
InfoMC got its start in 1995 by launching an enterprise platform to manage all clinical and core administration functions for a Philadelphia-based managed behavioral health organization. Shortly after, the platform was expanded to also support Employee Assistance Programs adding community referrals and scheduling. This solidified InfoMC’s position in the world of behavioral healthcare for years to come.


InfoMC got its start in 1995 by launching an enterprise platform to manage all clinical and core administration functions for a Philadelphia-based managed behavioral health organization. Shortly after, the platform was expanded to also support Employee Assistance Programs adding community referrals and scheduling. This solidified InfoMC’s position in the world of behavioral healthcare for years to come.
Inspired by his vision of improving healthcare, InfoMC CEO, JJ Farook, saw significant value in expanding beyond our behavioral health solution to create a whole-person, integrated care platform. By 2013, this led InfoMC’s transition to providing a cloud-based care management software, utilization management software and care coordination solution – supporting behavioral, physical and community-based services – known as the Incedo™ Healthcare Management System.
How It’s Going
Today, our client base of Managed Behavioral Health and Employee Assistance organizations has successfully expanded to include partnerships with Medicare Advantage Plans, Managed Medicaid, MLTSS and Specialty Plans who use Incedo to holistically manage care and services for their members through an integrated solution that includes:
Utilization Management for medical, behavioral and pharmacy
Care Management and care coordination to address physical, behavioral and social health drivers
Enhanced provider and care team communication and collaboration
CMS regulatory requirements and reporting
Over 26 million members are currently supported in better health with Incedo.
our leadership team
Designed to Improve the Whole Health Status of Individuals
The solution provides an integrated person-centered medical management platform that enhances interactions between plan, member, and provider to positively impact a member’s health and health outcomes.
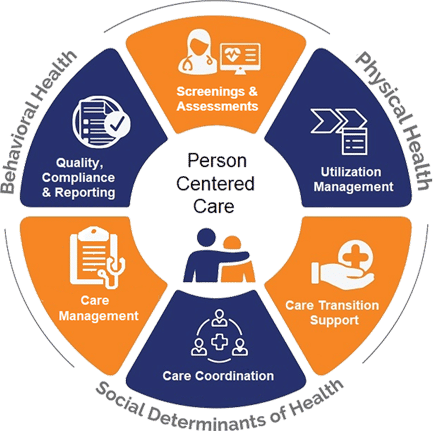
Achieve Better Quality, Clinical and Cost Outcomes
InfoMC’s solution uses a “whole-person” care approach that promotes quality, efficient and effective care with actively engaged members.
We have specifically designed our software to deliver operational efficiencies and improve outcomes by optimizing automation, streamlining workflows and putting valuable information in the hands of the care team, all in the pursuit of value-based care.


Our Difference



Customer Story
Learn how Doctors HealthCare Plans partnered with InfoMC just 45 days prior to their target go-live date, launched on time, and became the fastest growing MA plan two years in a row. Leveraging Incedo’s fully integrated medical management platform, Doctors continues to expand its footprint in highly a competitive market, having earned market distinction for offering innovative programs to their members.
InfoMC is proud to be a part of the Doctors Healthcare Plans success story.





